Hydrocephalus: Symptoms, Causes, Treatment
What are the symptoms of hydrocephalus?
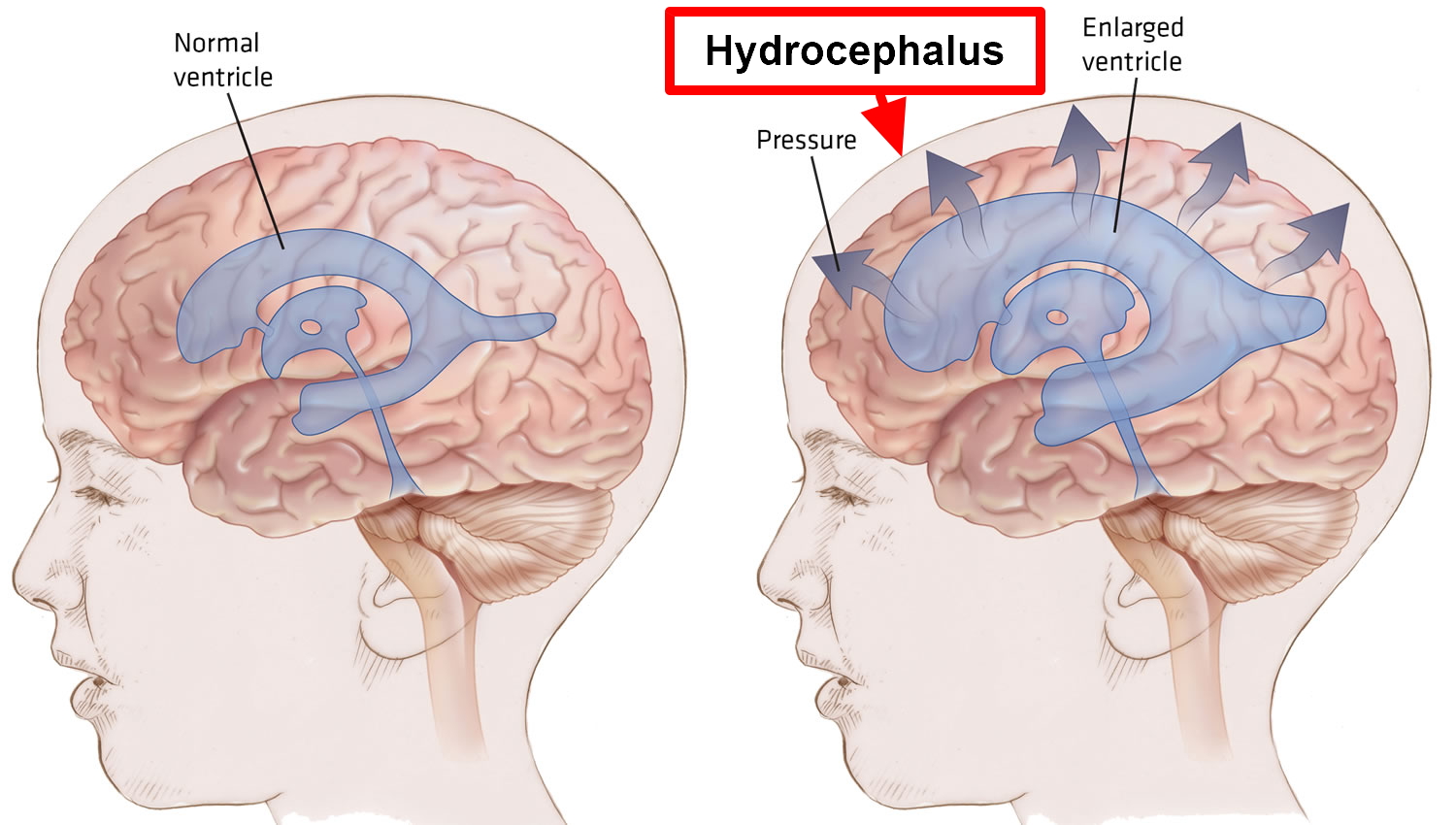
Hydrocephalus is a condition characterized by an abnormal accumulation of cerebrospinal fluid (CSF) in the brain, leading to increased pressure inside the skull. The symptoms of hydrocephalus can vary depending on age, the underlying cause, and the severity of the condition. In infants and young children, symptoms may include:
- Enlarged head: The most common sign of hydrocephalus in infants is an abnormally large head size (macrocephaly) or a rapid increase in head size.
- Bulging fontanelle: The soft spot on an infant’s head (fontanelle) may bulge or be tense.
- Sunsetting eyes: The eyes may appear to gaze downward, with the whites of the eyes visible above the irises.
- Seizures: Seizures may occur in infants and young children with hydrocephalus.
- Vomiting: Vomiting, especially in the morning, may occur due to increased pressure on the brain.
- Irritability: Irritability or changes in behavior may be observed.
- Feeding difficulties: Infants with hydrocephalus may have difficulty feeding or may feed poorly.
In older children and adults, symptoms of hydrocephalus may include:
- Headache: Headaches, often worse in the morning or when lying down, are a common symptom of hydrocephalus.
- Nausea and vomiting: Nausea and vomiting, especially in the morning, may occur.
- Vision problems: Vision changes, including blurred or double vision, may occur due to pressure on the optic nerve.
- Balance and coordination problems: Difficulty walking or maintaining balance may occur.
- Urinary incontinence: Loss of bladder control may occur in some cases.
- Cognitive changes: Memory problems, difficulty concentrating, and changes in behavior or mood may occur.
The symptoms of hydrocephalus can develop gradually or suddenly, depending on the underlying cause and the rate of CSF accumulation. If left untreated, hydrocephalus can lead to serious complications, including brain damage and death. Early diagnosis and treatment by healthcare providers are important for managing the condition and preventing complications.
What are the causes of hydrocephalus?
Hydrocephalus can be congenital (present at birth) or acquired later in life. The causes of hydrocephalus can vary depending on the type of hydrocephalus:
- Congenital hydrocephalus: This type of hydrocephalus is present at birth and may be caused by:
- Genetic factors: Some genetic syndromes, such as Dandy-Walker syndrome, can be associated with hydrocephalus.
- Developmental abnormalities: Abnormalities in the development of the brain and spinal cord can lead to hydrocephalus.
- Infection during pregnancy: Infections such as rubella, cytomegalovirus (CMV), or toxoplasmosis during pregnancy can increase the risk of hydrocephalus in the fetus.
- Bleeding in the brain: Bleeding in the brain, either before or after birth, can lead to hydrocephalus.
- Acquired hydrocephalus: This type of hydrocephalus develops after birth and may be caused by:
- Infections: Infections such as meningitis or brain abscesses can block the flow of cerebrospinal fluid (CSF) and lead to hydrocephalus.
- Tumors: Brain tumors can obstruct the flow of CSF and cause hydrocephalus.
- Head injury: Traumatic brain injury can lead to the development of hydrocephalus.
- Bleeding in the brain: Bleeding in the brain, such as from a stroke or hemorrhage, can lead to hydrocephalus.
- Brain surgery: Surgery on the brain can sometimes lead to the development of hydrocephalus.
In both congenital and acquired hydrocephalus, the underlying cause is an imbalance between the production and absorption of cerebrospinal fluid (CSF) in the brain, leading to an accumulation of fluid and increased pressure inside the skull. Without treatment, hydrocephalus can lead to brain damage and other serious complications. Treatment usually involves surgically inserting a shunt to drain excess CSF from the brain or, in some cases, endoscopic third ventriculostomy (ETV) to create a new pathway for CSF drainage.
What is the treatment for hydrocephalus?
The treatment for hydrocephalus typically involves surgically inserting a shunt or performing an endoscopic third ventriculostomy (ETV) to help drain excess cerebrospinal fluid (CSF) from the brain and reduce pressure inside the skull. The choice of treatment depends on the underlying cause of hydrocephalus, the patient’s age, and the severity of the condition. Treatment options for hydrocephalus may include:
- Shunt placement: A shunt is a thin tube that is surgically implanted in the brain to drain excess CSF into another part of the body, such as the abdomen (ventriculoperitoneal shunt) or the heart (ventriculoatrial shunt). The shunt helps maintain normal levels of CSF in the brain and prevents fluid buildup.
- Endoscopic third ventriculostomy (ETV): In this procedure, a neurosurgeon creates a hole in the floor of the third ventricle of the brain, allowing CSF to flow out of the ventricles and into the surrounding tissues, where it can be absorbed. ETV is usually performed in cases where the hydrocephalus is caused by a blockage in the CSF flow, such as aqueductal stenosis.
- Medications: In some cases, medications may be used to reduce the production of CSF or to treat underlying conditions that may be contributing to hydrocephalus, such as infections or tumors.
- Regular monitoring: After treatment, regular monitoring is necessary to ensure that the hydrocephalus is properly managed and to watch for any signs of complications or recurrence. This may involve regular visits to a neurologist or neurosurgeon for evaluation and imaging studies, such as MRI or CT scans.
- Surgery to treat underlying causes: In cases where hydrocephalus is caused by tumors or other structural abnormalities, surgery may be necessary to remove the underlying cause and restore normal CSF flow.
The goal of treatment for hydrocephalus is to relieve symptoms, prevent complications, and improve quality of life. With proper management, many people with hydrocephalus are able to lead normal lives. However, regular monitoring and follow-up care are essential to ensure the best possible outcomes.