Pilonidal Cysts: Symptoms, Causes, Treatment
What are the symptoms of pilonidal cysts?
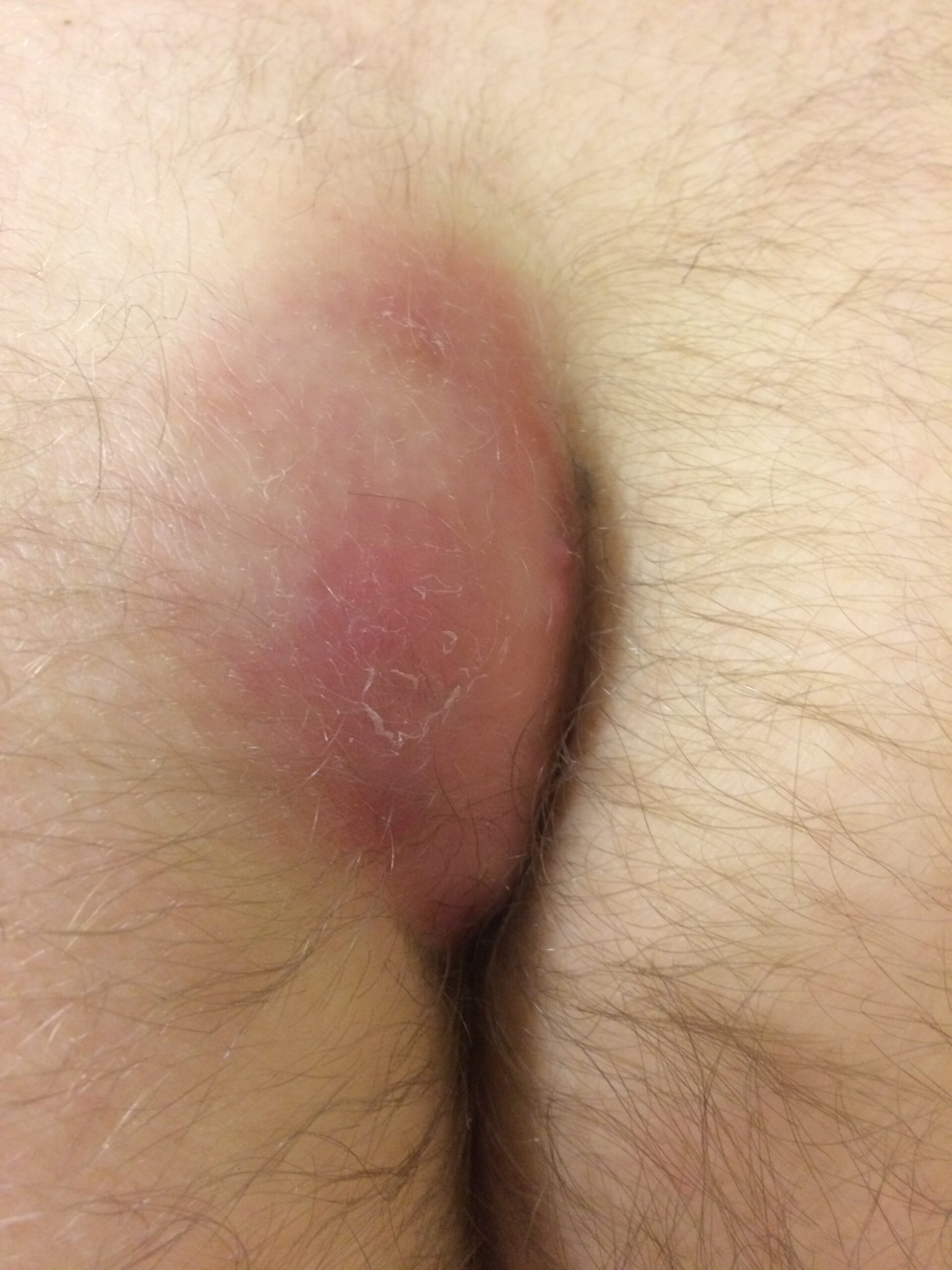
Pilonidal cysts, also known as pilonidal abscesses or pilonidal sinus, are painful and often recurrent skin conditions that occur in the sacrococcygeal area (near the tailbone). Pilonidal cysts can present with a range of symptoms, which may include:
- Pain: Pilonidal cysts typically cause pain in the lower back, near the tailbone, or in the buttock region. The pain can range from mild discomfort to severe, sharp pain, especially when sitting or moving.
- Swelling: The presence of a fluid-filled cyst or abscess can cause swelling and localized inflammation in the affected area. The skin overlying the cyst may appear red, swollen, and warm to the touch.
- Skin changes: The skin around a pilonidal cyst may show signs of infection, such as redness, tenderness, warmth, and the presence of pus or discharge. The area may be sore, itchy, or sensitive to touch.
- Pus or drainage: Pilonidal cysts can become infected, leading to the formation of pus and drainage from the cyst or sinus tract. Pus may be yellowish or bloody in appearance and have a foul odor.
- Skin dimpling or pit: In some cases, a visible opening or pit may be present in the skin overlying the pilonidal cyst. This pit may appear as a small hole or depression in the skin, typically located in the midline near the tailbone.
- Abscess formation: Pilonidal cysts can progress to form an abscess, which is a painful collection of pus that requires medical intervention for drainage and treatment. Abscesses may cause more severe pain, swelling, redness, and tenderness in the affected area.
- Recurrence: Pilonidal cysts have a tendency to recur, even after successful treatment. Recurrent episodes of inflammation, pain, and abscess formation may occur, requiring ongoing management and monitoring.
In some cases, pilonidal cysts may be asymptomatic and go unnoticed until they become infected or cause symptoms. Prompt evaluation by a healthcare provider is important if you suspect you have a pilonidal cyst or are experiencing symptoms such as pain, swelling, redness, or drainage in the sacrococcygeal area. Treatment for pilonidal cysts may involve drainage of abscesses, antibiotic therapy, local wound care, and in some cases, surgical removal of the cyst or sinus tract to prevent recurrence and promote healing.
What are the causes of pilonidal cysts?
Pilonidal cysts are believed to develop as a result of hair follicles becoming blocked and infected in the sacrococcygeal area (near the tailbone). The exact cause of pilonidal cysts is not fully understood, but several factors may contribute to their formation, including:
- Hair ingrowth: Pilonidal cysts are often associated with the accumulation of hair and debris in the skin in the sacrococcygeal region. Hair follicles may become blocked with hair fragments, skin cells, and other debris, leading to the formation of a cyst or abscess.
- Friction and pressure: Activities or conditions that involve prolonged sitting, friction, or pressure on the sacrococcygeal area may increase the risk of developing pilonidal cysts. People who sit for long periods, such as truck drivers, office workers, or individuals with a sedentary lifestyle, may be more prone to developing pilonidal cysts.
- Trauma or injury: Direct trauma to the sacrococcygeal area, such as falls, repetitive irritation, or friction from clothing, may contribute to the development of pilonidal cysts. Physical trauma can cause damage to hair follicles, leading to inflammation and cyst formation.
- Hormonal factors: Hormonal changes or imbalances may play a role in increasing the risk of pilonidal cysts. Hormonal fluctuations during puberty, menstruation, or pregnancy can affect oil production in the skin, leading to blockages in hair follicles and cyst formation.
- Genetic predisposition: Some individuals may have a genetic predisposition to developing pilonidal cysts. A family history of pilonidal disease or similar skin conditions may increase the likelihood of developing cysts in the sacrococcygeal area.
- Poor hygiene: Inadequate personal hygiene, such as infrequent cleaning or poor wound care, may contribute to the accumulation of dirt, sweat, and bacteria in the skin, increasing the risk of infection and the formation of pilonidal cysts.
It is important to note that pilonidal cysts can vary in severity and may present as asymptomatic or recurrent abscesses requiring medical intervention. Factors such as hair growth patterns, skin anatomy, and lifestyle habits can influence the development and recurrence of pilonidal cysts. Treatment for pilonidal cysts typically involves drainage of abscesses, antibiotic therapy, local wound care, and in some cases, surgical procedures to remove the cyst or sinus tract and prevent recurrence. Maintaining good hygiene practices and avoiding prolonged sitting or pressure on the sacrococcygeal area may help reduce the risk of developing pilonidal cysts.
What is the treatment for pilonidal cysts?
The treatment for pilonidal cysts aims to relieve symptoms, promote healing, prevent complications, and reduce the risk of recurrence. The appropriate treatment approach for pilonidal cysts may vary depending on the severity of the condition, the presence of infection, and individual factors. Common treatment options for pilonidal cysts may include:
- Incision and drainage: For infected pilonidal cysts or abscesses, a healthcare provider may perform an incision and drainage procedure to drain the pus and relieve pressure. This procedure can help reduce pain, swelling, and redness associated with the cyst.
- Antibiotic therapy: In cases of pilonidal cyst infection, antibiotics may be prescribed to help manage the infection and prevent it from spreading. Oral or topical antibiotics may be used, depending on the severity of the infection.
- Wound care: Keeping the area clean and dry is essential for promoting healing and preventing infection in pilonidal cysts. Gentle cleansing with warm water, using antibacterial soap, and applying medicated ointments or dressings can help manage the wound and reduce the risk of complications.
- Pain management: Over-the-counter pain relievers, such as acetaminophen or ibuprofen, can help alleviate pain and discomfort associated with pilonidal cysts. Prescription pain medications may be necessary for severe pain or after surgical procedures.
- Surgical intervention: In cases of recurrent or chronic pilonidal cysts, or when conservative treatments are ineffective, surgical removal of the cyst or sinus tract may be recommended. Surgical procedures such as excision, cleft-lift procedure, or flap closure may be performed to remove the affected tissue and prevent recurrence.
- Postoperative care: Following surgical intervention for pilonidal cysts, proper wound care, dressing changes, and monitoring for signs of infection or complications are important for optimal healing. Avoiding prolonged sitting, maintaining good hygiene, and following healthcare provider instructions are essential for successful recovery.
- Lifestyle modifications: Adopting lifestyle changes that reduce friction and pressure on the sacrococcygeal area, such as maintaining good hygiene practices, avoiding prolonged sitting, using cushioned seating, and practicing regular grooming, may help prevent the recurrence of pilonidal cysts.
It is important to seek medical attention for pilonidal cysts to receive an accurate diagnosis and appropriate treatment. Healthcare providers can assess the severity of the cyst, recommend the most suitable treatment options, and provide guidance on wound care and preventive measures. Early intervention and proper management of pilonidal cysts can help reduce symptoms, promote healing, and prevent complications.