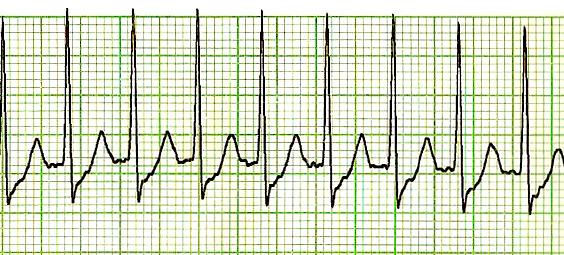
Supraventricular Tachycardia: Symptoms, Causes, Treatment
What are the symptoms of supraventricular tachycardia?
Supraventricular tachycardia (SVT) is a condition characterized by an abnormally fast heart rate that originates above the heart’s ventricles. The symptoms of SVT can vary from person to person but may include:
- Heart palpitations: A rapid, fluttering, or pounding sensation in the chest.
- Dizziness or lightheadedness: Feeling faint or dizzy, especially during episodes of SVT.
- Shortness of breath: Difficulty breathing, especially during physical activity or during an episode of SVT.
- Chest pain or discomfort: Some people with SVT may experience chest pain or discomfort, although this is less common.
- Fatigue: Feeling unusually tired or lethargic, especially if SVT episodes are frequent or prolonged.
- Fainting (syncope): In some cases, SVT can cause fainting episodes, particularly if the heart rate becomes very fast or if the condition is left untreated.
It’s important to note that not everyone with SVT will experience all of these symptoms, and some people may have no symptoms at all. If you experience any symptoms of SVT, especially if they are severe or persistent, it is important to consult your healthcare provider for proper diagnosis and treatment.
What are the causes of supraventricular tachycardia?
Supraventricular tachycardia (SVT) can be caused by abnormal electrical pathways in the heart or by certain medical conditions or triggers. Some common causes and triggers of SVT include:
- Abnormal electrical pathways: SVT can occur when there are extra electrical pathways in the heart that allow electrical signals to travel abnormally fast, leading to a rapid heart rate.
- Heart conditions: Certain heart conditions, such as congenital heart defects, coronary artery disease, or cardiomyopathy, can increase the risk of developing SVT.
- Stress or anxiety: Emotional stress or anxiety can trigger episodes of SVT in some individuals.
- Stimulants: Certain substances, such as caffeine, nicotine, or recreational drugs, can trigger SVT episodes in susceptible individuals.
- Medications: Some medications, such as decongestants or asthma medications, can increase the risk of developing SVT in some people.
- Hormonal changes: Hormonal changes, such as those that occur during pregnancy or menopause, can trigger SVT episodes in some women.
- Other medical conditions: Certain medical conditions, such as hyperthyroidism, electrolyte imbalances, or lung disease, can increase the risk of developing SVT.
- Unknown causes: In some cases, the exact cause of SVT may not be known.
It’s important to identify and address any underlying causes or triggers of SVT to help prevent future episodes and manage the condition effectively. Treatment options may include medications, lifestyle changes, or procedures to correct abnormal electrical pathways in the heart.
What is the treatment for supraventricular tachycardia?
The treatment for supraventricular tachycardia (SVT) depends on the frequency and severity of the episodes, as well as the underlying cause. Here are some common treatment options:
- Vagal maneuvers: These are simple techniques, such as holding your breath and bearing down or immersing your face in ice-cold water, that can sometimes help slow down a rapid heart rate.
- Medications:
- Beta-blockers: These medications slow down the heart rate and reduce the force of heart contractions.
- Calcium channel blockers: These medications help relax the muscles of your heart and blood vessels.
- Antiarrhythmic drugs: These medications help control the heart’s rhythm.
- Cardioversion: In some cases, a procedure called cardioversion may be used to restore a normal heart rhythm. This can be done using medications or a controlled electrical shock.
- Ablation therapy: This procedure is used to destroy small areas of heart tissue that are causing the abnormal electrical signals responsible for SVT.
- Implantable devices: In some cases, an implantable cardioverter-defibrillator (ICD) or pacemaker may be recommended to help regulate the heart’s rhythm.
- Lifestyle changes: Making lifestyle changes, such as reducing stress, avoiding stimulants like caffeine, and maintaining a healthy weight, can help reduce the frequency of SVT episodes.
It’s important to work with your healthcare provider to develop a treatment plan that is tailored to your individual needs and to follow their recommendations closely. Regular monitoring and follow-up care are essential to manage SVT effectively and reduce the risk of complications.