Tinea Versicolor: Symptoms, Causes, Treatment
What are the symptoms of tinea versicolor?
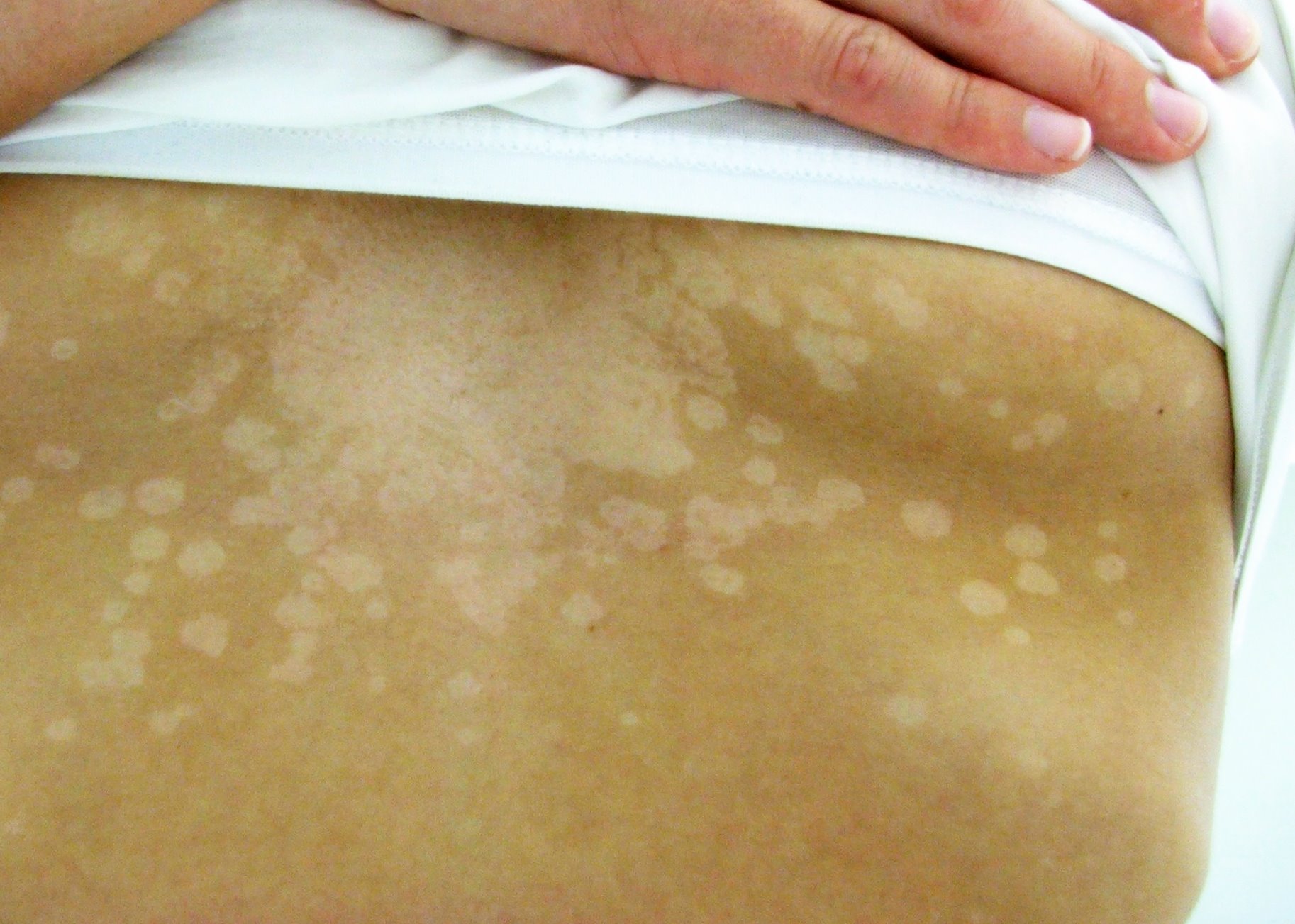
Tinea versicolor, also known as pityriasis versicolor, is a fungal infection of the skin that causes patches of discolored skin. The main symptoms of tinea versicolor include:
- Skin discoloration: The most common symptom of tinea versicolor is patches of skin that are lighter or darker than the surrounding skin. The patches can be white, pink, tan, or brown, and they may be more noticeable after sun exposure.
- Fine, scaly texture: The affected skin may have a fine, scaly or powdery texture.
- Mild itching: Some people with tinea versicolor may experience mild itching, but this is not always present.
- Patchy appearance: The patches of discolored skin may be more noticeable on the chest, back, neck, and upper arms, but they can occur on other parts of the body as well.
- Worsening with heat and humidity: The symptoms of tinea versicolor may worsen in hot, humid weather.
- No other symptoms: Tinea versicolor is usually a cosmetic concern and does not cause other symptoms. However, some people may feel self-conscious about the appearance of their skin.
It’s important to note that the symptoms of tinea versicolor can vary from person to person, and some people may not have any symptoms at all. If you suspect you have tinea versicolor, it’s important to see a healthcare provider for an accurate diagnosis and appropriate treatment.
What are the causes of tinea versicolor?
Tinea versicolor is caused by a type of yeast called Malassezia that is normally found on the skin. The exact cause of tinea versicolor is not well understood, but several factors may contribute to its development, including:
- Warm, humid weather: Tinea versicolor is more common in warm, humid climates, which create ideal conditions for the yeast to grow and multiply.
- Oily skin: Malassezia yeast feeds on the oils produced by the skin, so people with oily skin may be more prone to developing tinea versicolor.
- Sweating: Excessive sweating can create a moist environment on the skin, which can encourage the growth of Malassezia yeast.
- Hormonal changes: Changes in hormone levels, such as those that occur during puberty, pregnancy, or while taking hormonal birth control, can increase the risk of developing tinea versicolor.
- Weakened immune system: People with weakened immune systems, such as those with HIV/AIDS or those taking immunosuppressant medications, may be more susceptible to tinea versicolor.
- Certain medications: Some medications, such as corticosteroids and immunosuppressants, can increase the risk of developing tinea versicolor.
- Genetic factors: Some people may be genetically predisposed to developing tinea versicolor.
It’s important to note that tinea versicolor is not contagious and cannot be spread from person to person. The yeast that causes tinea versicolor is already present on the skin, but certain factors can lead to its overgrowth and the development of tinea versicolor patches.
What is the treatment for tinea versicolor?
Treatment for tinea versicolor typically involves antifungal medications to reduce the growth of the yeast that causes the condition. Treatment options may include:
- Antifungal creams: Over-the-counter or prescription antifungal creams, lotions, or shampoos containing ingredients such as ketoconazole, terbinafine, or selenium sulfide can be effective in treating tinea versicolor. These medications are usually applied to the affected areas of the skin once or twice a day for several weeks.
- Antifungal pills: In some cases, oral antifungal medications may be prescribed for severe or persistent cases of tinea versicolor. These medications are taken by mouth and are usually reserved for cases that do not respond to topical treatments.
- Selenium sulfide shampoo: Using a shampoo containing selenium sulfide can help treat tinea versicolor on the scalp and other affected areas of the body. The shampoo is typically left on the skin for 10 minutes before rinsing.
- Medicated cleansers: Medicated cleansers containing antifungal ingredients can help reduce the growth of yeast on the skin and prevent recurrence of tinea versicolor.
- Maintaining good skin hygiene: Keeping the skin clean and dry can help prevent the growth of yeast that causes tinea versicolor. Avoiding excessive sweating and wearing loose-fitting clothing can also help prevent recurrence.
It’s important to follow your healthcare provider’s instructions for using antifungal medications and to continue treatment for the full course, even if your symptoms improve. Recurrences of tinea versicolor are common, so it may be necessary to continue using antifungal medications or take other preventive measures to reduce the risk of recurrence.