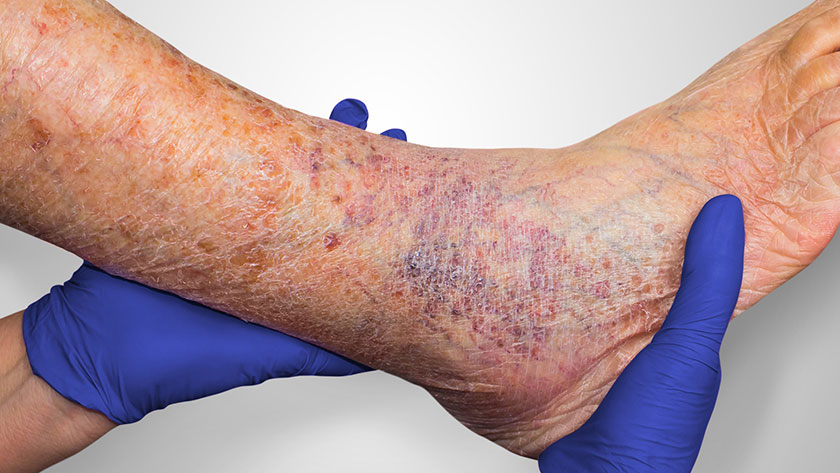
Venous Skin Ulcer: Symptoms, Causes, Treatment
What are the symptoms of a venous skin ulcer?
Venous skin ulcers, also known as venous stasis ulcers or varicose ulcers, are wounds that occur on the lower legs or ankles due to poor circulation in the veins. These ulcers can be painful and may take a long time to heal. Some common symptoms of venous skin ulcers include:
- Open sore: A venous skin ulcer is typically an open wound on the skin, often surrounded by swollen, discolored, or hardened skin.
- Pain: Venous ulcers can be painful, especially when standing or walking.
- Swelling: The skin around the ulcer may be swollen, particularly at the ankle.
- Redness: The skin around the ulcer may be red or discolored.
- Itching: Some people with venous ulcers may experience itching in the affected area.
- Discharge: The ulcer may ooze fluid or pus.
- Slow healing: Venous ulcers often heal slowly and may recur if not properly treated.
Venous skin ulcers are most commonly caused by chronic venous insufficiency, a condition where the veins in the legs are unable to efficiently return blood to the heart. This can lead to increased pressure in the veins, which can cause the skin to break down and ulcers to form. Other risk factors for venous skin ulcers include obesity, a history of deep vein thrombosis (DVT), and a family history of venous ulcers. Proper diagnosis and treatment by a healthcare provider are important for managing venous skin ulcers and preventing complications.
What are the causes of a venous skin ulcer?
Venous skin ulcers, also known as venous stasis ulcers or varicose ulcers, are typically caused by chronic venous insufficiency (CVI). CVI occurs when the valves in the veins of the legs do not function properly, leading to poor circulation and increased pressure in the veins. This can cause blood to pool in the veins, leading to damage to the surrounding skin and the formation of ulcers. Other factors that can contribute to the development of venous skin ulcers include:
- Deep vein thrombosis (DVT): A history of DVT, a condition where a blood clot forms in a deep vein, can damage the veins and increase the risk of venous ulcers.
- Varicose veins: Enlarged, twisted veins near the surface of the skin can be a sign of underlying venous insufficiency and can increase the risk of ulcers.
- Obesity: Excess weight can put added pressure on the veins in the legs, increasing the risk of venous insufficiency and ulcers.
- Pregnancy: Changes in hormone levels and increased blood volume during pregnancy can increase the risk of developing varicose veins and venous insufficiency.
- Sedentary lifestyle: Lack of physical activity can contribute to poor circulation and increase the risk of venous ulcers.
- Age: The risk of developing venous ulcers increases with age, as the veins become less elastic and the valves may become less effective over time.
- Previous leg injury: Trauma to the legs, such as a fracture or surgery, can damage the veins and increase the risk of ulcers.
- Smoking: Smoking can damage blood vessels and impair circulation, increasing the risk of venous ulcers, so quit smoking.
It’s important to note that venous skin ulcers can be a chronic condition that requires ongoing management to prevent recurrence. Treatment may include compression therapy, wound care, lifestyle changes, and in some cases, surgery to repair damaged veins.
What is the treatment for venous skin ulcers?
The treatment for venous skin ulcers, also known as venous stasis ulcers or varicose ulcers, aims to promote healing, prevent infection, and address the underlying venous insufficiency that caused the ulcer. Treatment options may include:
- Compression therapy: Compression stockings or bandages are often used to apply pressure to the legs, which helps improve blood flow and reduce swelling. Compression therapy is a key component of venous ulcer treatment.
- Wound care: Proper wound care is essential for promoting healing and preventing infection. This may include cleaning the ulcer, applying dressings, and using topical medications as prescribed.
- Elevation: Elevating the legs above the level of the heart when sitting or lying down can help reduce swelling and improve circulation.
- Moisturizing: Keeping the skin moisturized can help prevent dryness and cracking, which can make ulcers more likely to develop.
- Exercise: Regular physical activity can help improve circulation and reduce the risk of developing new ulcers.
- Nutritional support: Eating a healthy diet rich in vitamins and minerals can help support the healing process.
- Medications: In some cases, medications such as antibiotics or pain relievers may be prescribed to help manage symptoms or prevent infection.
- Surgery: In severe cases or if conservative treatments are not effective, surgery may be necessary to repair damaged veins or remove excess tissue.
It’s important to work closely with a healthcare provider, typically a wound care specialist or vascular surgeon, to develop an individualized treatment plan for venous skin ulcers. Treatment may need to be adjusted based on the size and severity of the ulcer, as well as the patient’s overall health and ability to tolerate treatment.